
10 The use of calcium hydroxide (Ca(OH) 2) dressing can reduce the flexural strength of dentine and microbial products themselves can degrade collagen. 10 There is a synergistic effect of ethylenediaminetetraacetic acid (EDTA) and NaOCl. A number of steps in the protocol of root-canal treatment have a negative effect on collagen including the use of sodium hypochlorite (NaOCl), with concentrations over 2% having more deleterious effects. 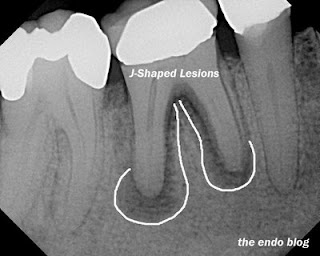
The process of endodontic treatment predominantly results in collagen depletion this affects the elasticity of the dentine and predisposes to fracture during shearing forces. However, nothing is reported in the literature in relation to parafunction and failure of endodontically treated teeth. 
Chewing forces are predominantly vertical, but in parafunction they can also be horizontal, 9 though in anterior teeth there is a much greater horizontal vector of force depending on the guidance on the anterior teeth. The relevance of loading forces may be more prudent in parafunctional patients as parafunctional loads can be six times the normal chewing force (1.5 to 7 kg) for an excess of 35 minutes in 24 hours, whereas normally teeth come together for chewing and empty swallows (eight minutes) for about 17.5 minutes every 24 hours. 8 The periodontal ligament may act as a protective feature. It is thought that proprioception is reduced by 30% after endodontic treatment as a result of pulpal nerves being involved in regulating masticatory load. Proprioception is also purportedly affected by endodontic treatment with higher pain threshold seen in non-vital teeth and therefore increased loading of non-vital teeth. 7 However, it must be remembered that most teeth requiring endodontic treatment have already suffered caries, cracks, trauma and previous restorations which may be the cause of weakness. 3, 4 Some have theorised that obtaining straight-line access may weaken adjacent cusps 5 others have suggested that post preparation removes radicular dentine, which weakens teeth 6 or that excess force during canal obturation causes tooth weakening. 3 It is the loss of the marginal ridges and occlusal isthmus that leads to weakening of teeth. 
2 In posterior teeth endodontic procedures were shown to reduce the stiffness of teeth by 5%, however, the presence of an occlusal restoration reduced stiffness by 20% and the presence of a mesio-occluso-distal restoration reduced tooth stiffness by 63%. In anterior teeth, no difference in fracture susceptibility of root-filled and non-root-filled anterior teeth has been shown. The changes in tooth architecture are often attributed to the access cavity preparation and removal of the vital tissues, supposedly rendering the tooth weaker and more susceptible to fracture. Although the effects are similar for both anterior and posterior teeth, the consequences are different due to the difference in tooth morphology and loading patterns. It is thought that endodontic treatment leads to 'weakening' of the remaining tooth structure as a result of various factors: changes in tooth architecture, changes in the properties of dentine and changes in proprioception. A root filled tooth is unlike a vital tooth due to the effect of endodontic treatment.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
